The concentration of refluxed acid is another important determinant of the degree of injury. These agents appear to have a synergistic effect, so reflux of acid and pepsin produces greater mucosal injury than reflux of acid alone. Hydrochloric acid and pepsin are the noxious agents most responsible for injuring esophageal mucosa. The severity of reflux disease also depends on the content of the refluxed material. In one study, 60% of patients with scleroderma who underwent endoscopy had evidence of reflux esophagitis. As a result, esophageal involvement by scleroderma often leads to severe esophagitis because of absent peristalsis and extremely poor clearance of peptic acid from the esophagus after reflux has occurred. Because the duration of reflux is related to the efficacy of esophageal clearance by peristalsis, dysmotility exacerbates reflux disease and increases the risk of developing esophagitis by prolonging exposure to refluxed acid. The severity of GERD depends not only on the frequency of reflux episodes but also on their duration. In most patients, however, these reflux episodes result not from a sustained decrease in resting sphincter pressure but from multiple transient LES relaxations that frequently occur at night.

GER occurs when lower esophageal sphincter (LES) pressure is decreased or absent, so the major barrier to reflux is lost. Reflux esophagitis is thought to be a multifactorial process related to the frequency and duration of reflux episodes, content of the refluxed material, and resistance of the esophageal mucosa. With double-contrast techniques, barium studies therefore have a major role in the evaluation of patients with GERD. Double-contrast esophagography is also a useful screening examination for Barrett’s esophagus. By permitting a more detailed assessment of the esophageal mucosa, however, double-contrast radiographic techniques have made it possible to detect superficial ulceration and other changes of mild or moderate esophagitis before the development of deep ulcers or strictures.
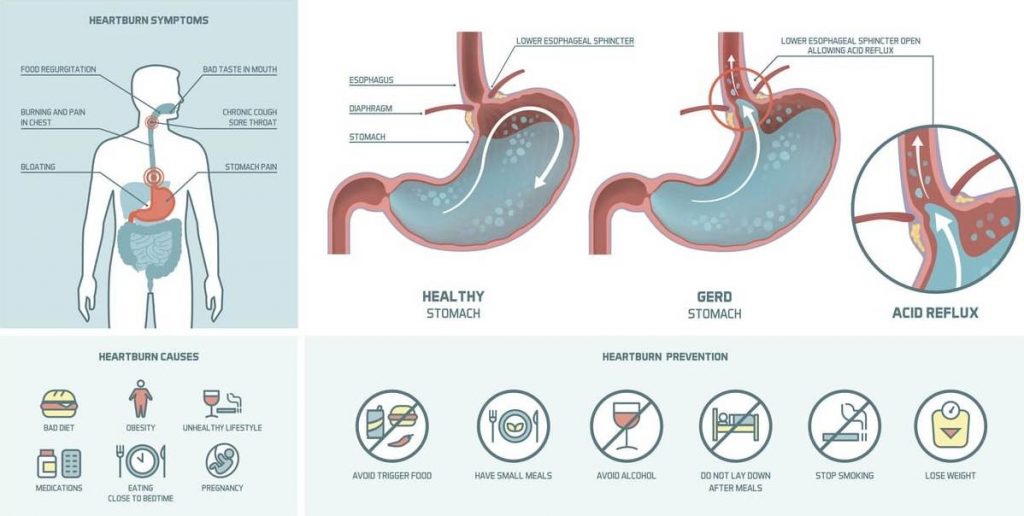
In the past, barium studies were advocated for patients with reflux symptoms primarily to show the presence of a hiatal hernia or gastroesophageal reflux (GER), detect complications such as deep ulcers or strictures, and rule out other organic or motor abnormalities in the esophagus that can mimic reflux disease. Gastroesophageal reflux disease (GERD) is the most common inflammatory disease involving the esophagus, with a prevalence of 10% to 20% in the West. Relationship Among Hiatal Hernia, Gastroesophageal Reflux, and Reflux Esophagitis
